The Functional Medicine Boom
The structural failures driving its rise, the research behind its results, and the accessibility problem nobody is talking about
Picture two people sitting in the same waiting room. Both have IBD. Both are about to receive dietary guidance grounded in the same clinical literature, developed from the same evidence base, delivered with the same confidence.
One of them also has diabetes.
IBD management often limits high-fiber, hard-to-digest foods and flags raw vegetables, whole grains, and legumes as common triggers. Diabetes management often leans on those same foods to stabilize blood sugar, improve satiety, and support metabolic health. For the person managing both, the guidance does not just fall short. It points in two directions at once.
This is not a rare case. Conflicts like this are common, under-discussed, and quietly absorbed by the millions of patients living inside them. Neither doctor is wrong, and neither guideline is inherently flawed. They are simply products of a system designed to treat one thing at a time, in a world where that is rarely how illness actually works.
The Single-Condition Illusion
Most people with a chronic condition are not managing just one. They are navigating several at once, receiving separate guidance for each, and trying to make it all work in the same body.
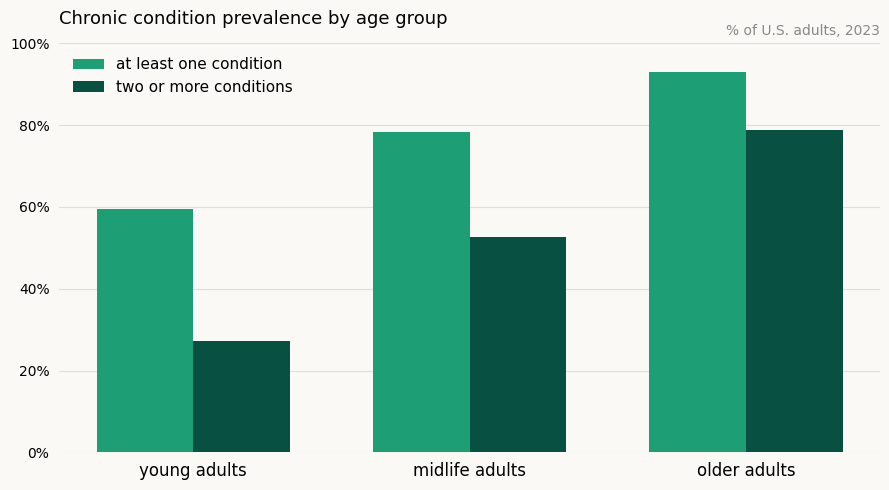
Source: CDC
Over 51% of American adults are managing two or more chronic conditions. Among older age groups, the rate of managing two or more conditions nearly matches the rate of having any condition at all. At that scale, isolated treatment protocols are not just incomplete. They are the wrong tool entirely.
The research meant to close that gap has its own problem. A PLOS One study reviewing 161 clinical trials found that in more than half of them, researchers did not record whether their participants had other conditions alongside the one being studied. Not whether those conditions changed the results. Just whether they were there at all. In many trials, patients with additional conditions were screened out before the study even began.
The problem is not only that guidelines are condition-specific. It is that the research underneath those guidelines often removes the very complexity that defines real chronic illness. Patients are left trying to reconcile advice that was never fully tested for lives like theirs. A system designed around the exception has spent decades treating it like the rule.
Where Patients Started Going
As chronic disease prevalence grew and patient dissatisfaction compounded, a parallel market was quietly building. Patients who felt unseen by conventional care began seeking out a model that treated the whole person rather than the presenting condition. Functional medicine stepped into that opening.
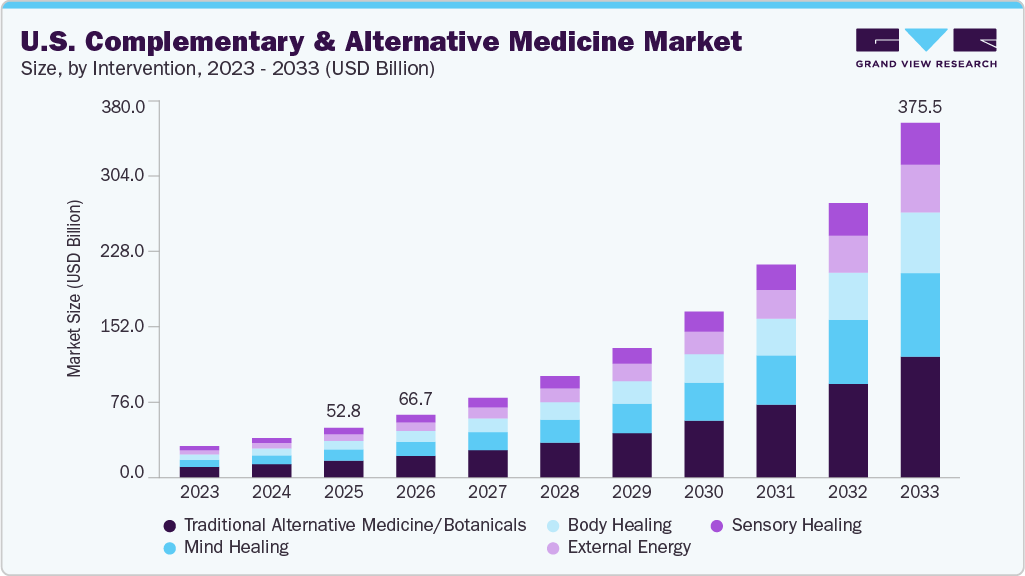
Source: Grand View Research
The Complementary and Alternative Medicine Market is projected to grow in the U.S. from $66.7 billion in 2026 to $375.5 billion by 2033, with a compound annual growth rate of nearly 28%. That is not a niche trend finding its moment. It is a reallocation of healthcare spending at a scale that reflects a deeper shift in the kind of care patients are looking for.
NIH research tracking complementary health use found adoption nearly doubled from 19.2% in 2002 to 36.7% in 2022, driven by patients seeking something conventional care was not offering. The reasons were consistent across every survey:
Root cause care over symptom management
Guidance personalized to their conditions and circumstances
Lifestyle treated as seriously as lab results
Functional medicine became the most organized expression of that demand. Longer appointments, individualized protocols, and a definition of health that extended beyond what a blood panel could capture. For patients who had spent years being told their labs looked fine while feeling anything but, that reframing did not just feel different. It felt like the first honest conversation they had been offered.
A Closer Look: The Cleveland Clinic Study
Functional medicine is still a relatively young field, which makes the research behind it worth examining carefully. The most rigorous test of the model to date came out of the Cleveland Clinic in 2019, published in JAMA Network Open.
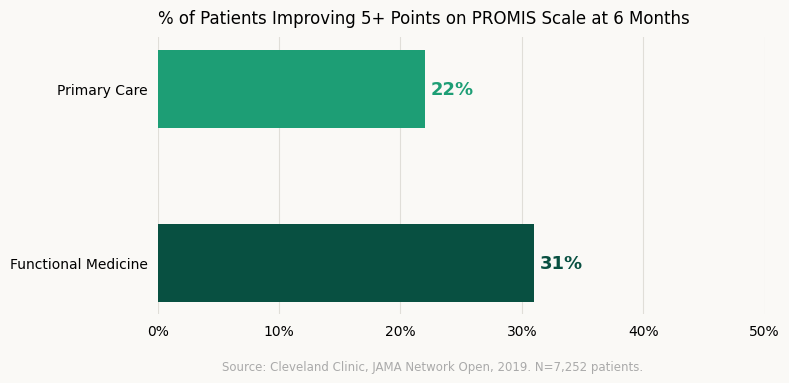
Researchers compared 1,595 patients treated at their Center for Functional Medicine against 5,657 patients in standard primary care. They measured outcomes across energy, pain, digestion, physical function, and emotional wellbeing using PROMIS, an NIH-validated assessment tool.
The results were surprising to some. Functional medicine patients were over 40% more likely to hit a clinically meaningful improvement threshold than their primary care counterparts at six months.
No single study settles a debate this complex, but this one was particularly hard to dismiss. Large sample size, NIH-validated outcome measures, a real primary care comparison group, and results that held up over time. It is the kind of institutional, peer-reviewed evidence that functional medicine has often been criticized for lacking. Then Cleveland Clinic provided it.
The Accessibility Issue
While functional medicine has shown tremendous promise early on, cost remains the largest barrier the field has yet to solve. This is the natural consequence of delivering highly personalized care through a system built for volume. Longer appointments and individualized protocols are exactly what makes functional medicine effective and exactly what makes it expensive.
Initial consultations typically run $300 to $500, with lab panels and diagnostic testing easily pushing total first-year costs into the thousands. Insurance rarely covers any of it, for a litany of reasons worth their own conversation. This means the people carrying the heaviest chronic disease burden are often times the ones least positioned to absorb what insurance will not.
Solving the access problem requires rethinking how personalized guidance gets delivered in the first place. The insight at the center of functional medicine, that recommendations should be built around who someone actually is, does not have to be gated behind an expensive clinical visit. The right data about a person and enough population-level research to find people who genuinely resemble them across age, medical history, and lifestyle context can surface the behavioral changes most likely to matter for that specific individual. This is guidance derived from real outcome patterns in real people with real complexity.
Lab results, blood panels, and microbiome testing do not lose their value in that model. They just stop being the price of admission. A tool that works without them is accessible to everyone. A tool that can incorporate them when available becomes more precise for the people who have them. Start with what someone can provide and get more specific as more information comes in. That is how you serve the full spectrum of people who need this kind of guidance, not just the ones who can already afford to know their biomarkers.
Takeaways
The numbers behind functional medicine's rise tell a story about unmet need more than they tell a story about alternative health. Here is what the research actually shows.
Over half of American adults manage two or more chronic conditions simultaneously, yet the clinical guidelines meant to help them were built around one condition at a time.
Complementary health adoption nearly doubled over two decades, driven by patients seeking care that conventional medicine could not keep up with.
The Cleveland Clinic's 2019 study found functional medicine patients were over 40% more likely to reach meaningful improvement than primary care patients at six months.
At $300 to $500 per visit with lab costs that can easily exceed thousands, personalized care remains a luxury for the patients carrying the heaviest burden.
Functional medicine identified the right problem: chronic care needs to account for the full person, not just the diagnosis in front of them. The work that remains is making that insight available to everyone, not just the patients who can afford to seek it out. The demand has been there for a long time. What is still being built is a way to meet it.